|
FA has the ability to visualize breakdown of the blood-retinal barrier (with the finding of “leakage” of extravasated fluorescein), but is limited in its ability to resolve the depth of specific signal abnormalities, and cannot visualize the deeper retinal capillary layers (ICP and DCP) due to blocked fluorescence 11, 12.Īn illustration of the retinal vascular plexuses in red (labeled on right) hand drawn on top of a histological section of the human retina showing anatomic layers (labeled on left) from spectral domain optical coherence tomography. Current clinical imaging of the ocular circulation has been dominated by fluorescein angiography (FA), a 2D imaging modality that was developed in the 1950’s that captures the fluorescence signal from intravenously injected dye in the retinal and choroidal circulation, and many retinal conditions are defined by their characteristic FA patterns. This organization of the retinal vascular plexuses has been confirmed in humans ex vivo using confocal microscopy 7, 8 and in vivo using speckle variance OCT 9 and adaptive optics confocal scanning laser ophthalmoscopy (AO-cSLO) 10 in research studies, technologies with a very narrow field of view and which are not widely available. The functional significance of the RPCP has been recognized due to its role supplying the densely packed nerve fiber layer (NFL) bundles in this region 4, 5, 6. The radial peripapillary capillaries have a unique anatomic organization because they run in parallel with the NFL axons, as opposed to the deeper vascular plexuses, which have a lobular configuration 4, 5. 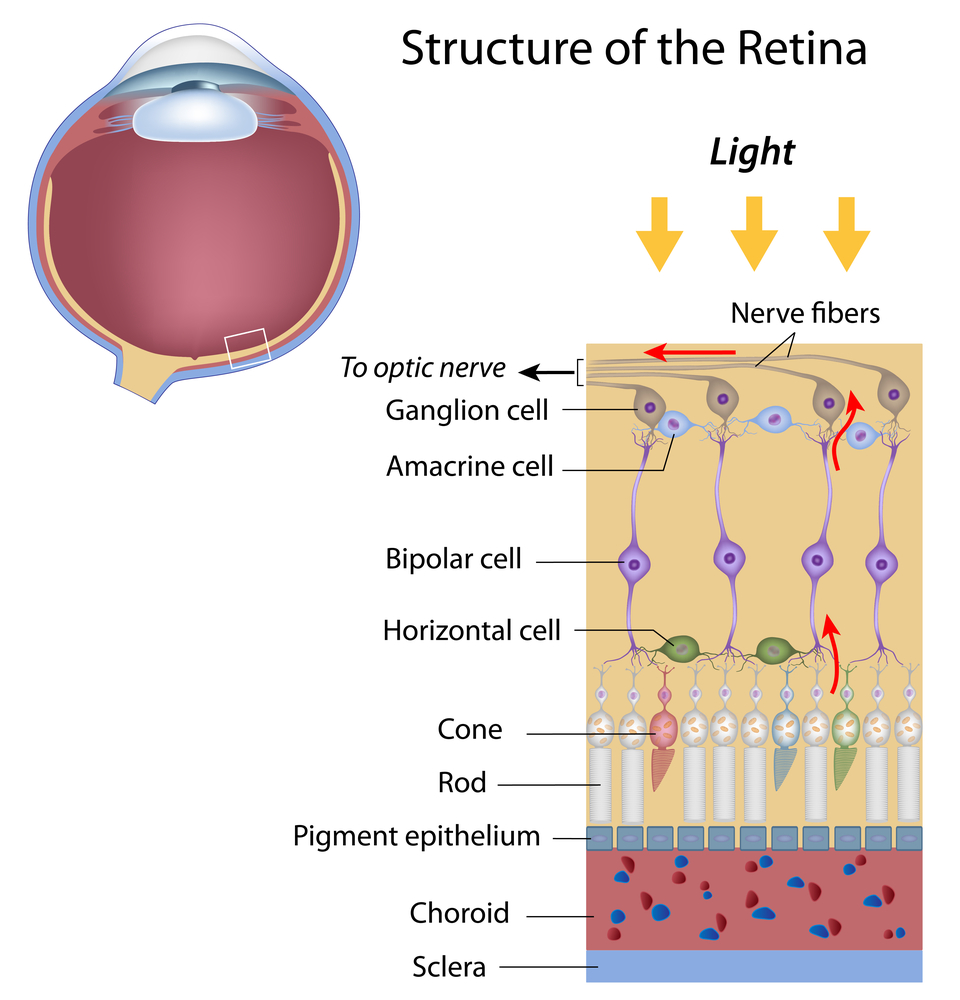
The fourth network is a regional layer called the radial peripapillary capillary plexus (RPCP). There are two deeper capillary networks above and below the inner nuclear layer (INL) referred to as the “intermediate” and “deep” capillary plexuses, or ICP and DCP, respectively, which are supplied by vertical anastomoses from the SVP 1, 2. The superficial vascular plexus (SVP) is supplied by the central retinal artery and composed of larger arteries, arterioles, capillaries, venules, and veins vessels primarily in the ganglion cell layer (GCL). From these early studies, we know that there are up to four retinal vascular networks in the macula ( Fig. Our current understanding of the retinal vascular networks developed from pioneering work on primate histology 1, 2. This could serve as a basis for future investigation of both normal retinal anatomy, as well as vascular malformations, nonperfusion, and neovascularization. Based on these data, we propose an improved system of nomenclature and segmentation boundaries for detailed 3-dimensional retinal vascular anatomy by OCTA. 
The vascular pattern in these retinal plexuses and interconnecting layers are consistent with previous histologic studies. Our investigation in normal human volunteers revealed the presence of 2 to 4 distinct vascular plexuses in the retina, depending on location relative to the optic disc and fovea. 
This novel technology allowed us to study the normal retinal vasculature in vivo with better depth resolution than previously possible. The projection-resolved (PR) OCTA algorithm improves depth resolution by removing projection artifact while retaining in-situ flow signal from real blood vessels in deeper layers. However, vascular depth discrimination is limited by superficial vessels projecting flow signal artifact onto deeper layers. Optical coherence tomography angiography (OCTA) is a noninvasive method of 3D imaging of the retinal and choroidal circulations.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
